Call for Evidence for Impact Assessment of the European Biotech Act Will Close June 11, 2025
The European Commission (EC) began a call for evidence on May 14, 2025, for an impact assessment of the European Biotech Act. The EC states that the overall objective is to improve the size and competitiveness of the biotechnology sector in the European Union (EU) while maintaining high safety standards. The new European Biotech Act will aim to ensure that the EU makes the most of the biotechnology revolution for the benefit of society, the environment, and the economy, while making it easier to develop and bring to market products across all biotechnology sectors in the EU. According to the EC, the European Biotech Act would address the following issues:
European companies have difficulty expanding within the single market because of “a complex regulatory framework that is perceived as slow and burdensome.” According to the EC, there are cases where implementation of the relevant EU regulatory framework diverges among EU member states, resulting in regulatory environments that are complex to navigate for companies and that can hinder the development or commercialization of biotechnology products. In addition, barriers at national or regional levels can further delay or hinder market entry.
The growth and development of biotechnology companies in Europe is hindered by market fragmentation, risk capital constraints, and scattered innovation support. EU companies lack sufficient access to risk-tolerant capital, and there is a lack of coordinated private and public investment to support the translation of innovation into products and the scaling-up of production for innovative biotechnology products.
The EC states that the EU does not tap into the full potential of its scale when it comes to pooling capacities to make it more competitive globally. Because national interests often lead to support for local companies, many biotechnology clusters exist throughout the EU. Some clusters are mostly of regional relevance, do not cover all the steps from laboratory to market, duplicate efforts at low scale, do not fully use their capacities, or have limited resources.
Manufacturing biotechnology products requires highly specialized equipment and a highly qualified and multidisciplinary workforce. According to the EC, in the EU, there is a mismatch between the labor supply and the biotechnology and biomanufacturing skills required.
Artificial intelligence (AI) and big data — including access to supercomputing capacity and to large, integrated, high-quality datasets — offer huge potential for all sectors underpinned by biotechnology, provided that appropriate safeguards are put in place.
The impact assessment will explore the following areas:
Speed and streamlining: “Time-to-market” is an essential parameter for the successful translation of innovation into commercial products. Where appropriate, the regulatory environment for biotechnology needs to be simplified, including the procedures for risk assessments. The aim is to facilitate and speed up the development and approval of biotechnology products and to bring them to the market faster and more easily, without compromising safety for health and for the environment or biosecurity standards. Best practices for accelerated time-to-market at EU, national, and regional levels need to be promoted.
Financing: Having access to sufficient capital is key to supporting the process of translating innovation into product development and the scaling-up of production capacities. Risk-tolerant capital is essential for the development of the biotechnology industry at seed phase, scale-up stage, and at later stages of development.
Scale: Tapping into the potential of the EU in terms of both scale of production and market size can help to ensure that companies thrive in Europe. Further options could be to look at possible support for the development, operation, governance, and coordination of biotechnology clusters or centers of excellence in the EU. The EC states that an open, competitive and at-scale business environment will be essential to keep the EU ahead in the global race.
Skills: Specific measures will be considered to improve the upskilling and reskilling of the workforce in the biotechnology area. This is to ensure that companies have access to adequately trained staff and to equip academic developers with the necessary entrepreneurial skills to create and grow a company.
Use of data and AI in the biotechnology sector: Access to data, storage services, and computing resources is essential for biotechnology research and innovation and for the development of AI tools and solutions to support the development of biotech products. According to the EC, having access to supercomputing capacity and AI testing facilities is essential to enable biotechnology companies and organizations to use data effectively. Targeted projects and tailored programs at the EU level have the potential to facilitate and push forward the development and adoption of digital solutions and AI in all biotechnology sectors.
Comments are due June 11, 2025. The EC plans a public consultation on the draft legislation in the fourth quarter of 2025, and to adopt final legislation in the third quarter of 2026.
McDermott+ Check-Up: June 6, 2025
THIS WEEK’S DOSE
Senate Begins Work on Reconciliation. Democrats prepared to file points of order to exclude certain provisions under the Byrd rule, while Republicans discussed key health provisions.
White House Sends Congress $9.4 Billion Rescissions Package. The package requests that Congress rescind $900 million in global health funding.
Senate HELP Committee Reviews Reauthorization of Over-the-Counter Monograph Drug User Fee Program. Discussion focused on layoffs at the US Food and Drug Administration (FDA) and how the agency can expedite over-the-counter medication development.
House Begins FY 2026 Appropriations Markups. The Subcommittee on Agriculture, Rural Development, FDA, and Related Agencies met to mark up its fiscal year (FY) 2026 bill.
HHS Releases FY 2026 Budget in Brief. The US Department of Health and Human Services (HHS) budget in brief requests $94 billion in discretionary funding, a $31 billion decrease from FY 2025.
CMS Rescinds 2022 EMTALA Abortion Guidance. The agency noted that the Emergency Medical Treatment and Active Labor Act (EMTALA) guidance did not reflect the current administration’s priorities.
FDA Declines to Appeal Ruling on LDT Regulation. A federal court previously struck down the laboratory-developed test (LDT) final rule, and the FDA declined to appeal within the given 60-day window.
Fired HHS Employees File Class Action Lawsuit. The federal case alleges that firings were based on incorrect personnel records.
CONGRESS
Senate Begins Work on Reconciliation. The Senate returned from its Memorial Day recess to begin consideration of HR 1, the One Big Beautiful Bill Act, the House-passed reconciliation package. Senate Majority Leader Thune (R-SD) aims to have a modified bill on the floor the week of June 23, 2025, with the goal of getting a final bill to President Trump’s desk by July 4, 2025. This week’s work occurred mostly behind the scenes. Senate committees of jurisdiction are not expected to hold markups; instead, committees of jurisdiction will release titles of the bill within their jurisdiction. The process started this week. The Senate Committee on Commerce, Science, and Transportation released its language that modifies the House’s artificial intelligence (AI) provisions, removing the 10-year state ban on AI regulation and amending funding language so that states would only be eligible for AI development grants if they do not enforce state laws regulating AI models. The Senate Finance Committee, with jurisdiction over Medicaid, taxes, and the Affordable Care Act (ACA), will likely be the last committee to release updated text. Majority Leader Thune noted that the Finance Committee title could be released as soon as next week.
Majority Leader Thune can lose no more than three Republicans to pass the bill. This week, more Republicans came out in opposition to certain Medicaid provisions, including the moratorium on provider taxes. Sens. Collins (R-ME), Murkowski (R-AK), Moran (R-KS), and Hawley (R-MO) are among those with concerns. On the conservative side, Sens. Paul (R-KY), Johnson (R-WI), Lee (R-UT), and Rick Scott (R-FL) continued to voice strong opposition unless the bill does more to cut federal spending and reduce the deficit. There has also been discussion about potentially including Medicare Advantage reforms to increase savings, although no explicit policies have been presented publicly. Senate passage will likely require a delicate balancing act, and afterward the bill must pass the House again. President Trump met this week with Senate Finance Committee Republicans, and Centers for Medicare & Medicaid Services (CMS) Administrator Oz is holding meetings in the Senate to hash out concerns and attempt to reach policies that can unite Republicans. The process to scrub the bill of provisions that don’t meet the Byrd rule is also ongoing. Republicans met with the Senate Parliamentarian this week, and Democrats likely will follow soon. (For a full explainer on the Byrd rule, read our +Insight).
On June 4, 2025, the Congressional Budget Office (CBO) released updated estimates for H.R. 1. CBO estimates that the bill would increase the deficit by $2.4 trillion. This figure is based on a $1.2 trillion reduction in federal spending offset by a $3.6 trillion decrease in revenue. CBO estimates that 10.9 million individuals would be uninsured in 2034. Of those, 7.8 million would lose Medicaid coverage, with others mainly losing coverage from changes to the ACA. CBO estimates that the ACA changes would result in gross benchmark premiums for ACA plans decreasing by an average of 12%. At the request of Senate Democrats, CBO released additional analysis that provides further details on health insurance loss and estimates that failure to extend the enhanced advance premium tax credits as part of H.R. 1 would lead to an additional 5.1 million Americans being uninsured in 2034.
White House Sends Congress $9.4 Billion Rescissions Package. The package asks for more than $9 billion of previously appropriated funding to be rescinded and is largely focused on foreign aid and the Corporation for Public Broadcasting. The package includes recissions of funding from health programs within the US Department of State and the US Agency for International Development (USAID). It requests rescission of $500 million in global health USAID funding that focuses on equity, family planning, and reproductive health within child and maternal health, HIV, and infectious disease activities. It also requests rescission of $400 million of President’s Emergency Plan for AIDS Relief (PEPFAR) funding. Congress has 45 days to act. Approval of the rescission package only requires a simple majority in the House, which will likely consider it next week. In the Senate, Appropriations Chair Collins (R-ME) has already stated concerns about PEPFAR cuts and noted her committee’s intention to examine the package.
Senate HELP Committee Reviews Reauthorization of Over-the-Counter Monograph Drug User Fee Program. During the hearing, Democrats focused on how workforce reductions at the FDA will impact agency operations, while supporting the development of over-the-counter (OTC) drugs. Republicans advocated for a more streamlined and efficient transition from prescription drugs to OTC medications, emphasized the need for regulatory oversight of international facilities, and encouraged use of an online dashboard to track the FDA’s progress. Jacqueline Corrigan-Curay, MD, acting director of the FDA’s Center for Drug Evaluation and Research, expressed her commitment to working with Congress to streamline the transition from prescription drugs to OTC medications.
House Begins FY 2026 Appropriations Markups. The House Appropriations Committee began subcommittee markups this week to discuss spending bills for FY 2026. The Subcommittee on Agriculture, Rural Development, FDA, and Related Agencies held its markup, during which it advanced its bill to the full committee by a party line vote. During the markup, Republicans stated that the bill would help reduce the federal deficit, while Democrats criticized the bill for cutting funding for the FDA and the Supplemental Nutrition Assistance Program. The full schedule of subcommittee and full committee markups can be found here.
ADMINISTRATION
HHS Releases FY 2026 Budget in Brief. Late on May 30, 2025, HHS released its budget request for FY 2026, known as a budget in brief. Some agencies and divisions within HHS also released congressional justifications that provide more information on funding requests. Additional justifications from other agencies and divisions are said to be forthcoming. The budget in brief follows the earlier release of the “skinny” budget and provides more detail on HHS priorities, including the agency’s restructuring. The document only includes discretionary funding requests and does not include legislative proposals that would impact mandatory programs such as Medicare or Medicaid. Administration officials indicate that mandatory funding requests are unlikely to be released before reconciliation is complete.
Highlights for HHS discretionary funding requests include:
$95 billion for HHS, a $31 billion decrease from FY 2025.
$14 billion for the new Administration for a Healthy America (AHA), which HHS estimates to be a $6 billion cut from current funding levels for all the programs that will be transferred to AHA. The budget in brief includes an overview of the programs from the Health Resources and Services Administration, the Centers for Disease Control and Prevention (CDC), the Substance Abuse and Mental Health Services Administration, and the Office of the Assistant Secretary for Health that would be part of AHA.
$3.1 billion for FDA, a $409 million cut compared to FY 2025.
$4.1 billion for CDC, a $550 million cut compared to FY 2025.
$27.5 billion for NIH, a $17 billion cut compared to FY 2025.
The budget notes that NIH would cap indirect cost rates for grants at 15%, a policy that NIH pursued earlier this year, is subject to ongoing litigation, and is likely to face scrutiny from lawmakers on both sides of the aisle.
$3.5 billion for CMS, a $673 million cut compared to FY 2025.
Read more in our +Insight.
CMS Rescinds 2022 EMTALA Abortion Guidance. The Biden administration released the HHS guidance in July 2022 in the wake of the US Supreme Court Dobbs decision that left regulation of abortion to the states. The now-rescinded guidance stated that EMTALA protects healthcare providers’ clinical judgement and any action they take to provide stabilizing care for emergency medical conditions, including ectopic pregnancy, complications of pregnancy loss, or preeclampsia. In a press release, CMS noted that it will continue to enforce EMTALA, including in emergency medical situations where the health of a pregnant woman or her unborn child are at risk, and indicated that the agency will rectify any legal confusion on this issue.
COURTS
FDA Declines to Appeal Ruling on LDT Regulation. In late March 2025, the US District Court for the Eastern District of Texas struck down the regulation finalized in May 2024 under the Biden administration that gave the FDA the authority to regulate LDTs. The district court found that the rule violated the Loper Bright standard because the FDA exceeded its statutory authority. The FDA was given a 60-day window to appeal the decision, which it declined to do. Therefore, the final rule remains without force. Although the FDA did not issue a statement on its decision, it follows previous actions by the Trump administration to limit agencies’ regulatory power outside of statutory authority. Read more about the March court decision here.
It remains to be seen if the Trump administration will take a new approach to LDT regulation or if lawmakers will re-introduce the VALID Act, which received bipartisan support in previous session of Congress and would require the FDA to regulate LDTs and other in vitro diagnostics.
Fired HHS Employees File Class Action Lawsuit. In yet another challenge to the HHS reductions in force, seven former HHS employees filed a case in the US District Court for the District of Columbia. The lawsuit claims that the personnel files used to justify firings had errors and inaccuracies, which HHS Secretary Kennedy has attributed to siloed human resources departments across the agency. The lawsuit notes that most employees fired during the April 2025 reduction in force could be eligible for this class action.
QUICK HITS
FDA Begins Agency-Wide AI Tool Use. FDA employees are using the generative AI tool Elsa in various internal projects, including clinical protocol reviews and scientific evaluations. The tool was launched before the original deadline of June 30, 2025, and FDA will expand the tool over time.
HHS Announces Heads of ASTP, OCR. Thomas Keane, MD, a radiologist, will serve as the assistant secretary for technology policy (ASTP) and national coordinator for health information technology. Paula Stannard worked for HHS during the first Trump administration and will serve as director of the HHS Office of Civil Rights (OCR).
FBI Opens Tipline for Reports of Gender-Affirming Care for Minors. The tipline seeks reports of any hospitals or clinics performing gender-affirming care for minors and follows HHS tips for whistleblowers.
CMS Announces Health Technology Initiatives. In line with CMS’s request for information on the healthcare technology ecosystem, the initiatives include building an interoperable national provider directory and modernizing Medicare identification processes.
House Passes SUPPORT Act Reauthorization with Bipartisan Support. The legislation would modify HHS substance use and mental health disorder programs and reauthorize various grant programs through FY 2030. It passed by a vote of 366 – 57, with the nays mostly from Freedom Caucus Republicans and Energy and Commerce Democrats.
James O’Neill Confirmed as HHS Deputy Secretary. The Senate confirmed O’Neill by a 52 – 43 party line vote. Once sworn in, he will be second in command at HHS.
House Oversight Committee Ranking Member Questions AI Use in MAHA Report. Acting Ranking Member Lynch (D-MA) requested information from HHS Secretary Kennedy by June 16, 2025, to assess whether the agency used AI to write the recently released MAHA report.
GAO Releases Report on Diagnostic Testing for Pandemic Threats. The US Government Accountability Office (GAO) report summarizes insights from a roundtable of 19 experts. GAO recommends that HHS develop and periodically update a national diagnostic testing strategy for infectious diseases and establish a national diagnostic testing forum.
NIH Requests Information on Agency AI Strategy. NIH requests information about specific topics and notes that there is a need for a unified, Office of the Director-level AI structure to build synergy across program silos, improve transparency, and accelerate research and development. Comments are due July 15.
CMS Rescinds Biden-era Medicaid SOGI Data Guidance. The now-rescinded guidance aimed to help states with collecting sexual orientation and gender identity (SOGI) information in Medicaid applications. The rescission notes that CMS no longer intends to collect this data from states.
NEXT WEEK’S DIAGNOSIS
Both chambers of Congress will be in session next week, with work on reconciliation expected to continue in the Senate. The Senate Appropriations Committee will discuss the NIH FY 2026 budget, and the House Energy and Commerce Health Subcommittee will examine US-made medicine and domestic supply chains. The House Committee on Appropriations will consider the Agriculture, Rural Development, FDA, and Related Agencies appropriations bill that advanced from the subcommittee this week.
A Final Rule Bites the Dust, Part II: FDA Gives up on Regulating LDTs as Medical Devices
As the song goes, the Food and Drug Administration’s (“FDA’s”) 2024 Final Rule regulating laboratory-developed tests (“LDTs”) as medical devices (“Final Rule”), is not merely dead—it’s really most sincerely dead.
Perhaps not for good, but for the foreseeable future, at least.
The FDA has let the clock run out on the 60-day time period to appeal the March 31, 2025, decision by the U.S. District Court for the Eastern District of Texas concluding that: 1) the FDA overstepped its authority, and 2) the LDT Final Rule of May 6, 2024, was unlawful. As we explained at that time, the Final Rule would have required virtually all clinical laboratories offering their own LDTs to comply with FDA expectations for medical device manufacturers in phases over a four-year period—with the first compliance deadlines set for May 2025.
The March 2025 opinion by Judge Sean D. Jordan vacated the controversial Final Rule a little more than a month before the first implementation deadlines were to take effect, and remanded the issue back to the FDA.
Now, absent an appeal, it is not likely that the last remaining option to salvage the Final Rule—i.e., congressional action—will happen in the current political climate.
As we explained at the time of its release, the 2024 Final Rule followed more than a decade of uncertainty as to the course of action the agency would take with respect to LDTs. When it came, the Final Rule escaped potential rollback by a future presidential administration as a “midnight rule” under the Congressional Review Act—yet threw clinical labs into nearly a year o
As we anticipated, the Supreme Court’s June 28, 2024, decision in Loper Bright Enterprises v. Raimondo—ending Chevron deference to agencies when interpreting ambiguous statutes—made it easier for entities to challenge both FDA authority and the validity of the agency’s Final Rule. The American Clinical Laboratory Association and the Association for Molecular Pathology filed suit in federal district court in Texas on May 29, 2024, and August 19, 2024, respectively.
But perhaps no one could have anticipated the extent to which the FDA itself has changed in the lifespan of the LDT Final Rule—with unprecedented staff cutbacks, changing policies and priorities, and a continued emphasis on deregulation at the federal level that is not likely to change until a future presidential administration rolls in. States, meanwhile, continue to regulate LDTs to some extent, and the FDA continues to have authority to regulate certain components of LDTs (such as reagents and collection devices), as well as in vitro diagnostics. While this particular chapter on LDTs has drawn to a close, we aren’t going anywhere—and we will continue to advise our lab clients on state as well as remaining federal compliance considerations.
Attorney Ann W. Parks contributed to this article
Ad Restrictions on HFSS Products in the UK to Take Effect on 5 January 2026, with Voluntary Compliance from Advertisers and Broadcasters from 1 October 2025
The UK Government has delayed the implementation of the Advertising (Less Healthy Food Definitions and Exemptions) Regulations 2024 (“Regulations”), which were due to come into force on 1 October 2025, in order to explicitly exempt ‘pure brand’ advertising from the Regulations. The Regulations will now come into force on 5 January 2026. However, despite this delay, advertisers and broadcasters have voluntarily committed to complying with the restrictions from 1 October 2025 (as originally planned).
In a letter addressed to the Government, representatives from the advertising industry stated their commitment not to run ads for specific, identifiable less healthy food or drink products. The letter was signed by key advertising bodies, such as the Advertising Association, ISBA, the IPA and IAB. The letter was also signed by major media organisations and broadcasters, including Channel 4, ITV, Sky and Reach plc, along with the Food and Drink Federation.
The Regulations will impose new restrictions banning ads for “identifiable” food and drinks that are high in fat, salt or sugar (“HFSS”) from being shown on TV before 9pm in the UK or at any time in online paid-for advertising. The aim of the Regulations is to reduce the exposure of HFSS marketing to children by restricting such advertising, with the forthcoming change following numerous governmental commitments regarding HFSS restrictions over the past few years.
What restrictions will be introduced?
The restrictions being introduced include:
a 9pm watershed for “identifiable” less healthy food and drink advertising on TV. This will also include all on-demand programme services (“ODPS”); and
the introduction of a complete ban on paid-for less healthy food and drink advertising online, including on non-Ofcom regulated ODPS.
The Regulations will apply to businesses involved or associated with the manufacture or sale of “less healthy” food or drink with 250 or more employees (which includes franchises) who pay to advertise HFSS products. Only HFSS products that are “identifiable” will be regulated.
Which products are covered by the Regulations?
HFSS products within the scope of the Regulations are those:
falling within one of the 13 product categories in the schedule to the Regulations;[1] and
scoring at least a certain number of points under the relevant Nutrient Profiling Model technical guidance .
To help businesses understand the types of products that may fall outside the scope of the Regulations, Department of Health and Social Care (“DHSC”) guidance provides a list of non-exhaustive exemptions (e.g. neither dried fruit snacks nor garlic bread are HFSS products).
There are also numerous exempt products that are already subject to separate regulations, which include (among others) infant formula, total diet replacement products, meal replacement products (which use an approved health claim) and food for special medical purposes.
Enforcement
The Regulations will be enforced by the Advertising Standards Authority (“ASA”) and Ofcom. Non-compliant businesses could face the following (among others):
enforcement notices and corrective action;
consumer and competitor complaints;
financial penalties where the business makes serious breaches; and/or
reputation damage, which may be incurred as result of the ASA (and the press) publicly reporting on any non-compliance.
Pure brand advertising
‘Pure brand’ advertising refers to advertising that focuses on promoting a brand’s overall identity and recognition, rather than specific product features or promotions. However, the ASA considered that it was not clear whether pure brand advertising was caught within the scope of the restrictions or not.
Following this, the DHSC published a number of statements to clarify its position regarding pure brand advertising. Ashley Dalton, Parliamentary Under-Secretary of State for Public Health and Prevention, stated on 22 May 2025 that “the Government intends to make and lay a Statutory Instrument (SI) to explicitly exempt ‘brand advertising’ from the restrictions. The SI will provide legal clarification on this aspect of the existing policy, as it was understood and agreed by Parliament during the passage of the Health and Care Bill. This will enable the regulators to deliver clear implementation guidance and mean that industry can prepare advertising campaigns with confidence”.
As such, businesses can still promote their brands insofar as any ads do not identify less healthy products and be exempt from the restrictions.
Next steps
With only months until the restrictions are introduced, businesses within the food and drink sector and those supplying them (such as advisors, agencies and consultancies) should familiarise themselves with the new advertising obligations and assess current product compliance using the nutritional scoring to determine how impacted they will be. With the ASA shaping its guidance so regularly, businesses should monitor updates to proactively ensure that they are keeping abreast of any developments. Businesses may also want to consider adapting their marketing strategy to promote healthier products or reformulating certain products so that they are no longer deemed “less healthy” and caught by the restrictions.
[1] These products include (among others): soft drinks (category 1); savoury snacks (category 2); breakfast cereals (category 3); confectionary (category 4); ice cream/lollies (category 5); cakes and cupcakes (category 6); sweet biscuits and bars (category 7); “morning goods”, which includes pastries and pancakes (category 8); desserts and puddings (category 9); sweetened yoghurt (category 10); pizza (category 11); chips and wedges (category 12); and ready meals, products ordered from a menu that are intended to be consumed as complete meal, breaded or battered seafood or meat product and sandwiches (category 13).
The authors wish to thank Royce Clemente for his contribution to this post.
Hot Topics in Employee Benefits: A Primer for In-House Lawyers
Employee benefits compliance has many traps for the unwary and is ever evolving. Below, we have provided a primer on current issues of importance in the employee benefits area to help in-house attorneys identify potential risks, mitigate them, and know when to call an outside ERISA lawyer.
1. What Is Old Is New: Get Your Health Plan Governance in Order
Employers that sponsor self-funded health plans have a host of complicated obligations. There are greater potential legal, regulatory, and fiduciary risks than in years past with managing health plans because of increased congressional legislation, increased Department of Labor (DOL) focus on group health plan compliance, and increased group health plan litigation, often by the same plaintiffs’ firms that have been suing 401(k) plans in fee litigation the past 20 years or more.
Employers should consider properly establishing a benefits committee, much like how they established committees for their retirement plans, that will serve to govern and oversee their employer-sponsored group health plans, especially those that are self-funded. A formal committee could help employers stay compliant, formalize their prudent decision-making process, and shift certain fiduciary liability to the benefits committee from the Board, thus insulating the Board from the underlying fiduciary decisions.
2. Stay Calm and Carry On: Mental Health Parity Non-Enforcement Policy Pauses Only Certain Requirements
Self-insured health plans must show that the plan does not include more restrictions on access to mental health benefits than on access to medical benefits. The law looks at both financial limits (e.g., coinsurance, copays, and deductibles) and other types of limits (e.g., pre-authorization requirements, provider network design, and prescription drug formulary design).
Beginning in 2021, plans were required to produce a written analysis of the non-financial limits, also known as non-quantitative treatment limitations (NQTLs), and the DOL has been actively auditing those analyses. Such audits have been time- and resource-intensive, given that the DOL has yet to approve an analysis without changes.
Late last year, the agencies released a final rule with details on the DOL’s expectations with respect to the NQTL analysis. They have since been sued for the rule, with the plaintiffs claiming overreach by the DOL. On May 15, 2025, the DOL stated that it would not enforce the final rule but would continue to enforce the statute and prior guidance.
Therefore, self-insured plans should continue to produce and update their NQTL analysis. We expect at least some continued audit activity, as well as the threat of private litigation.
3. To Report or Not to Report, That Is the Question: Florida Data Request to Self-Insured Plans Under Pharmacy Benefits Management Law
Several states have recently enacted laws designed to increase oversight of pharmacy benefit managers (PBMs) and limit certain PBM practices. Many of these laws impose reporting obligations on PBMs and the plans and employers with which they contract. While some of these laws exempt self-funded group health plans from their reach, recognizing that states are generally preempted from regulating such plans under ERISA, others explicitly include self-funded group health plans within their reach. For example, Florida’s Prescription Drug Reform Act includes “self-insured employer health plans” in its definition of “pharmacy benefits plan or program”—the category of plans to which the law applies.
This year, Florida’s Office of Insurance Regulation issued data requests under the PBM law, asking PBMs and group health plans to submit a broad range of prescription drug data, including participants’ names, dates of birth, prescriptions filled, and doctors visited. For sponsors of self-funded health plans, these data requests and similar requests made by other state agencies raise questions regarding both ERISA preemption and Health Insurance Portability and Accountability Act (HIPAA) obligations.
We expect that these questions may soon be answered through litigation, but in the meantime, employers with self-funded plans should work with counsel to evaluate these requests on a case-by-case basis. In some instances, the requested data may be minimal, and the state laws may fall outside of ERISA’s broad preemption protection. In other cases, where states request sweeping, specific data, such requests might be preempted by ERISA, especially where sharing the information would violate HIPAA.
4. If You Didn’t Document It, It Didn’t Happen: Takeaways from Cunningham v. Cornell University
On April 27, 2025, the U.S. Supreme Court ruled in Cunningham v. Cornell University that a plaintiff can allege that a transaction between a plan and a “party in interest,” such as a plan service provider, is a “prohibited transaction” under ERISA even if the plaintiff doesn’t directly allege that the transaction was unreasonable or unnecessary. Why did the Supreme Court conclude a plaintiff doesn’t have to allege something specifically wrong, especially where transactions between plans and plan service providers are common? The Court took a textualist approach and concluded that ERISA’s structure puts the burden on the plan fiduciary to prove the transaction was necessary and reasonable, and because of this, a plaintiff need not plead “unreasonableness” in its complaint. As the Court conceded, the result is that the bar to get past a motion to dismiss is lowered, making it more difficult for plans to avoid costly litigation for weak—if not downright meritless—prohibited transaction claims. Recognizing that this may be problematic for plans, the Supreme Court urged lower courts to use other tools at their disposal to weed out meritless claims sooner rather than later, such as additional pleadings or the threat of shifting plan legal fees to a plaintiff.
So, what can a prudent plan administrator take away from a case about technical ERISA pleading standards? The clearer a fiduciary’s prudent process for selecting and compensating a plan service provider, the better. Clear documentation of the fiduciary’s process, such as in committee meeting minutes (preferably, vetted by experienced counsel), makes it more likely that a court will see the prudence a fiduciary has exercised from the get-go, before individuals have to defend their efforts in depositions.
5. How Well Is Your Wellness Plan?
HIPAA’s wellness program rules provide an exception to its general rule that prohibits an employer from determining premiums or benefits based on a health factor. Employers offering wellness programs should be mindful of ongoing challenges to health-contingent programs. These programs require participants to satisfy a standard related to a health factor to earn a reward. Health contingent programs can be outcomes-based or activity-only programs. While many of the requirements apply to both programs, challenges—and litigation—focus on health-contingent programs that are outcomes-based. These programs require employers to allow a “reasonable alternative standard” for meeting the requirements, regardless of whether it is medically inadvisable for a participant to try to meet the standard, or if meeting the standard is unreasonably difficult due to a medical condition. Cases focus on the availability of, or communication related to, a “reasonable alternative standard.”
Employers offering these plans should review their communications ahead of open enrollment season to make sure reasonable alternative standards are disclosed in all printed and electronic communications. Employers should also ensure that they are, in fact, offering a reasonable alternative standard as well as ensuring payment is made for any retroactive periods while the standard is being met.
6. Don’t You Forget About Me: Cybersecurity Guidance Applies to All Employee Benefit Plans
In April 2021, in the wake of a rash of phishing and hacking incidents that resulted in the theft of retirement funds, the DOL issued cybersecurity guidance for plan sponsors, plan fiduciaries, record keepers, and plan participants. Recognizing the vast assets being held in private-sector pension and defined contribution plans without sufficient vigilance, protections, and accountability, these assets may be at risk from both internal and external cyber threats.
The guidance issued by the DOL includes Tips for Hiring a Service Provider, Cybersecurity Program Best Practices, and Online Security Tips. However, it was heavily focused on ways to protect retirement plan data and the financial assets in retirement accounts, leading many to the misconception that the guidance didn’t extend to the data maintained by the plan sponsors, plan fiduciaries, and the contractors and vendors for health and welfare plans.
As cybercrime evolved and hackers began to use malware and ransomware, health care data became an increasingly attractive target because the services that health care organizations and their IT systems support keep people alive and healthy. Hackers appreciated that there was little tolerance for allowing health care systems to remain offline, making it more likely a ransom will be paid, creating the perfect storm and magnifying the value of health care data to cybercriminals. Breaches by large vendors made it abundantly clear that, in a digital world, the need for strong cyber hygiene transcends all boundaries, prompting the DOL to issue an update in November 2024 to the cybersecurity guidance to confirm that it applies to all ERISA plans.
No Man Is an Island: The Great Cannabis Debate
Most of the annual state legislative sessions have ended or are nearing an end, and it would be an understatement to say that the hemp industry has ever experienced a more widespread and seemingly coordinated effort to roll back consumable hemp programs. In some states, those reforms were dramatic. Others, substantial but not existential. Add to that the fact that Congress will eventually address hemp’s federal legal status in the next Farm Bill, and it is certainly understandable if hemp stakeholders believe they and their futures are on unsteady ground.
No man is an island,
Entire of itself;
Every man is a piece of the continent,
A part of the main.
The cannabis industry as a whole – and that includes marijuana, industrial hemp, and consumable hemp, just to name the most popular varietals – is in vulnerable position. Although it may appear so in retrospect, progress is rarely linear. Of course, growing a new industry always has certain fits and starts that can make it feel like a slog, but the cannabis industry has generally been successful in pushing the stone up the hill over the last two decades. But on the heels of that success, progress is looking less certain than it has in years.
A cornerstone of cannabis the industry and a fundamental tenet that has led to billions in investments is that things will continue to get better. Hope — a dangerous thing or the best of things? Are we sure about that fundamental tenet now?
The problems are numerous, and they are coming from inside and outside the industry. From outside, there is a sizeable portion of Americans who simply do not want cannabis products in the marketplace. While our readers probably disagree with this position, I recognize it to be at least honest opposition to a core philosophy. And Big Alcohol and Tobacco have reasons to keep out competition in the space. But it’s from inside the industry that may come the most insidious threat to its growth.
If a clod be washed away by the sea,
Europe is the less,
As well as if a promontory were:
As well as if a manor of thy friend’s
Or of thine own were.
In the end though, I believe infighting between marijuana and hemp operators is slowly diminishing the legitimacy of the plant rather than fighting for its growth in an equitable system.
I represent marijuana companies, consumable hemp companies, industrial hemp companies, and countless companies that aren’t in the cannabis space but seek counsel on how to live and work in a world where cannabis exists but their government hasn’t provided sufficient assurances for how to address cannabis issues.
I’m not picking sides here or arguing that hemp and marijuana operators should get along while both sides get a raw deal. If you’re a marijuana operator who thinks it’s bogus that someone can sell a product that – to the consumer – appears identical but without the punishing regulation, taxation, and expense, I agree with you. If you’re a hemp operator who believes they could sell their product in a competitive market if they could just escape the fog of the current federal and state regulatory landscape, I agree you should have the chance to compete with regulated marijuana.
Any man’s death diminishes me,
Because I am involved in mankind.
Texas has almost 10% of the country’s population and just banned consumable hemp. And to what end? To bolster Texas’ anemic medical cannabis program? Nope, still in the doldrums. Alabama just substantially limited its consumable hemp program while its medical program remains trapped in a protracted court battle. Tennessee just limited its hemp program, and it doesn’t even have a medical program. California? Don’t get me started.
Although I understand that many who have been in the marijuana business for two decades may feel differently, I believe we are in the equivalent of the stone ages when it comes to unlocking the potential of the cannabis plant. If we take off the shackles of overregulation and punitive tax policies that cut off the lifeblood of growth, we can have something at least approaching a fair market where companies can compete on a level playing field.
John Donne finishes his masterpiece with the following line that gives me chills every time I read it or hear it spoken:
Therefore, send not to know
For whom the bell tolls,
It tolls for thee.
Is this a warning? A prediction? Perhaps. But maybe it’s meant to motivate, to galvanize, and to encourage cooperation and a shared effort towards a common goal. I’d like to think that.
Conclusion
In the cannabis world, as in life, no man is an island. None of us will stand if we cause others to fall for reasons of shortsightedness, greed, or pettiness. For if we choose those paths, we will not need to ask for whom the bell tolls. But if we choose the greater course, where cannabis operators lift each other up instead of pulling each other down, we all just might have a chance to hear the chorus of bells ringing in our collective success.
Thanks for stopping by.
Listen to this article
CODEX ALIMENTARIUS: Main Outcome of the 44th Committee on Methods of Analysis and Sampling (CCMAS44)
The 44th session of the Codex Alimentarius Committee on Methods of Analysis and Sampling (CCMAS44) successfully addressed all topics on its agenda. CCMAS44 endorsed methods of analysis from commodity standards and recommended approval of others e.g., on chocolate, chocolate products and other cocoa-based products, fruits juices and nectars, fish products, follow-up formulas, food grade salt. CCMAS44 held intense discussions on methods of analysis for the protein content in quinoa and on the method for the determination of the moisture content in whey powder. CCMAS44 agreed also to establish an expert group under the auspice of the IFU to inform the work on the methods proposed for fruit juices and nectars. CCMAS44 finally agreed on rounded numeric performance criteria for the determination of nitrate and nitrite ions in food matrices. CCMAS44 decided also to start working on methods for the identity of “sugars and honey”. It also endorsed the method discussed during the last CCNFSDU44 meeting on dietary fiber with a further question back to CCNFSDU with a proposed amendment to a more comprehensive footnote. CCMAS44 adopted a comprehensively amended information document about sampling plans (with an entire new part 3 on Bayesian sampling plans) to inform the implementation of the current guidelines on sampling. CCMAS44 advanced the work on a consolidated list of methods for the presence of allergens that would be subject to another intersessional work. CCMAS44 re-established EWGs (including one to advance the harmonization of names for principles in the general standard of methods of analysis) and agreed to convene a working group in person immediately prior its CCMAS45 session (2026) [ii].
See more information available about CCMAS44 working documents quoted in this article [iii], as well as in the official report of the CCMAS44 meeting [iv]. Codex standards, guidelines, codes of practices and related miscellaneous texts quoted in this article are readily and freely available [v].
ENDORSEMENT OF METHODS OF ANALYSIS AND SAMPLING AND REVIEW OF METHODS INCLUDED IN THE GENERAL STANDARD FOR METHODS OF ANALYSIS (CXS 234, 2024 version)
Methods applicable cocoa products and chocolate; fish and fishery products; foods for special dietary uses; fruit juices and nectars; milk and milk products; and miscellaneous products such as dried meat and food grade salt
CCMAS44 agreed to (i) endorse all the methods and amended methods resulting from the work of pre-session VWG and an in-Session WG (IWG as summarized in CCMAS44’s CRD02 Rev.1 working document); (ii) revoke and retype the methods, as included in Appendix II of CCMAS44 report); (iii) inform the CCNFSDU that the methods of analysis submitted by it to CCMAS were forwarded for adoption by CAC48 and all the relevant methods of analysis be revoked consequentially. CCMAS44 agreed to re-establish its EWG on methods chaired by Canada (and not customarily by Australia), for further consideration on (a) cocoa products and chocolate; (b) foods for special dietary uses; and (c) fruit juices and nectars. CCMAS44 praised the work of Dr Richard Coghlan (Australia), as the outgoing chair of the EWG, VWG and IWG. CCMAS44 also agreed to re-establish a Physical Working Group (PWG) on methods endorsement led by the USA and co-led by Hungary, Japan and Uruguay to meet immediately prior to CCMAS45, to (a) consider all methods of analysis and sampling submitted by Codex Committees for endorsement, (b) the outcomes of the work of the EWGs on methods including retyping of the ISO 1871 method for determining protein in quinoa (see further below); the proposals on the workable packages on chocolate and cocoa-based products as well as on sugars and honey, and any other matters referred by other Codex Committees or submitted by Members and Observers.
CCMAS44 concluded favorably its work on methods applicable to (a) cocoa products and chocolate; (b) fish and fishery products; (c) foods for special dietary uses; (d) fruit juices and nectars; (e) milk and milk products; and (f) miscellaneous products such as dried meat and food grade salt. CCMAS44 did not propose changes to existing methods already included in CXS 234 applicable to (a) cereals, pulses and legumes and derived products; (b) fruit juices and nectars; (c) milk and milk products; and (d) miscellaneous products (e.g., dried meat and food grade salt). CCMAS44 also revoked methods as consequential changes from other adopted for the same standardized food [vi].
In order to advance the technical discussions on the remaining work package of methods in fruit juices and nectars, CCMAS44 agreed to convene an expert group under the auspices of the International Fruit and Vegetable Juices and Nectars Association (IFU) to (a) determine the ranges of parameters relevant for quality and authenticity; (b) determine the range of measurements or maximum LOD; (c) evaluate the list of endorsed methods included in CXS 234 and those listed in the commodity standard CXS 247 (2024 version) ; (d) determine/consider if the presently endorsed methods are still appropriate and “fit-for-purpose” to control the “quality and authenticity” of fruit juices; (e) determine/consider if any of the presently endorsed methods should be revoked and eliminated from CXS 234 and CXS 247; (f) assess whether any new method(s) could be considered by the CCMAS endorsement working group in the future, for addition to CXS 234 for the general provision of juice “quality and authenticity”; and (g) collate relevant validation data for any new procedures that CCMAS could consider in the future. In particular, the expert group shall identify clearly which methods should be maintained in CXS 234, revoked, or replaced. Codex Members were invited in contributing to this work by contacting directly IFU and nominate nationally relevant fruit juice experts to participate eventually to the work of that IFU-led expert group, in their individual capacity. CCMAS44 praised the coordinating work ensured by Dr David Hammond [vii] at IFU.
With regards the work package on methods for chocolate and chocolate products and other cocoa-based products, CCMAS44 agreed to re-establish an EWG chaired by Serbia and co-chaired by USA to continue reviewing the relevant methods listed. With regards to the work package of relevant methods for sugars and honey, CCMAS44 agreed to establish an EWG chaired by Uruguay to review these methods applicable to sugars and honey. Both EWGs should submit their report sufficiently in advance to CCMAS45.
As examples of methods endorsed, CCMAS44 agreed to retain the method for determination of amino acid nitrogen in fish sauce, AOAC 920.04 and AOAC 920.03, in CXS 234. CCMAS44 endorsed AOAC 935.47 and AOAC 937.09B as Type III methods. CCMAS44 agreed to transfer the method for the determination of sodium chloride in food grade salt as described in the Standard for food grade salt (CXS 150) with editorial amendments to CXS 234. CCMAS44 also agreed with an update to the hyperlink in the footnote referencing the method for iodine in food grade salt in CXS 234. In addition, CCMAS44 agreed to transfer the related sampling plan to CXS 234. CCMAS44 noted that the sampling plan was currently incompatible with the provision for sodium chloride and would require further review and agreed that such review could be taken up later under the work on the review of sampling plans and inform CCFA accordingly. CCMAS44 also noted the editorial amendment to the principle for the example methods AOAC 2015.06 / ISO 21424 |IDF 243 that meet the numeric performance criteria for copper in milk fat products and agreed to the removal of ISO 5738 | IDF 76 and AOAC 960.40 as example methods. All relevant commodity committees will be informed accordingly.
CCMAS44 further requested CCNFSDU to consider (a) whether it would be appropriate to develop numeric performance criteria (NPC) for methods of analysis for Type II and Type III methods; or (b) develop additional methods for follow-up formula to align with those for infant formula for common provisions (see Part 3.2 of Appendix II of CCMAS44 report). With regard to the recommendation for CCNFSDU to consider developing NPC, the chair of the VWG clarified that CCMAS’s preference was for committees to consider this approach. CCMAS44 noted that this approach would provide flexibility for countries to choose methods that meet these criteria. This approach was in accordance with the Procedural Manual that preference should be given to set NPC. CCMAS44 further agreed that the name and format for principles for the corresponding methods for infant formula included in CXS 234 would not be aligned with those agreed for follow-up formula at this stage pending ongoing discussion on the harmonization of names and format for principles. It was noted that CCNFSDU was also in the process of reviewing all methods for provisions in standards under their purview to assess their fitness-for-purpose and to identify additional/replacement methods, or other corrections.
Dietary fibre reference in Table 6 of CXS 234 “Methods of analysis for dietary fibre: Guidelines for use of nutrition and health claims (CXG 23, 2013 version): Tables of conditions for claims”
CCMAS44 endorsed the methods proposed by the outcome of the EWG and VWG (as presented in CCMAS44 CRD02 Rev.1 working document), together with the footnote proposed by CCNFSDU44 which reads “Isolated, purified, and/or synthetic fibres captured by AOAC 2022.01/ICC Standard 191/AACC 32-61.01 that do not meet the Codex definition of dietary fibre in the Guidelines on nutrition labelling (CXG 2-1985) should be subtracted from the final measurement, where deemed appropriate by competent authorities.” CCMAS44 also agreed to request CCNFSDU to clarify whether the footnote was only applicable to the methods AOAC 2022.01/AACC 32-61.01/ICC Standard No. 191. If not, the footnote should then apply to all methods for dietary fibers included in Table 6 of CXS 234, or a subset of these methods listed in that Table 6. Should CCNFSDU agrees, then CCMAS would delete the footnote applied only to AOAC 2022.01/AACC 32-61.01/ICC Standard No. 191.
CCNFSDU was further asked to consider a proposed amendment to the current footnote 2 included in Table 6 of CXS 234. Such proposed amendment would address the concerns raised that the footnote forwarded by CCNFSDU should be consistently applied to all methods in CXS 234, Table 6. Should CCNFSDU agree to amend footnote two, then the footnote forwarded by CCNFSDU to accompany AOAC 2022.01/AACC 32.61.01/ICC Standard No. 191 could then be deleted. The recommended additional phrase to existing footnote 2 is shown in bold as follows: « Two issues are left for national authorities: to include monomeric units 3-9 and which isolated or synthetic compounds have physiological benefit. (Refer to the Guidelines on nutrition labelling (CXG 2-1985)). Isolated, purified, and/or synthetic fibres captured by the analysis that do not meet the Codex definition of dietary fibre in CXG 2-1985 should be subtracted from the final measurement, where deemed appropriate by competent authorities. »
SPECIFIC DISCUSSIONS ON SOME METHODS
Determination of the protein content in quinoa products (conforming to CXS 333, 2020 version)
This agenda was very much disputed. CCMAS44 however agreed to retain the method for determining protein in quinoa already in CXS 234 as a Type IV method (method ISO 1871), noting the reservation of Peru. CCMAS44 requested the re-established PWG on endorsement to consider retyping of ISO 1871 method for determining protein in quinoa based on the information provided in CCMAS44’s CRD19, referring to a comprehensive comparative analytical work performed by several national metrological institutes based in Latin America in this matter. Brazil also suggested an extension of Extension of the ISO 20483 method to quinoa offered as an alternative method. It was suggested that the necessary validation studies could be performed and discussed again within ISO to determine if this method could be extended from cereals and pulses to a pseudocereal such as quinoa. ISO indicated that a decision to extend ISO 20483 to quinoa should be subject to a formal request according to ISO procedures. In that regard, it was also noted that ISO might even end up validating a dedicated method (to Quinoa) instead of extending the existing ISO 20483 to Quinoa [viii].
Determination of the moisture content in whey powders (conforming to CXS 289, 2022 version)
CCMAS44 agreed to forward the 102NP method with the footnote as amended in paragraph 41 to CAC48 for adoption as a Type IV method (Appendix II, Part 1.5), for whey powder, on an exceptional basis, in line with Section 3.9 (v) of the information document “Comprehensive guidance for the process of submission, consideration and endorsement of methods for inclusion in CXS 234” and to make the consequential amendments to Appendix XI of CXS 234 (2024 version).
Determination of the particle size of milling products using sieve analysis for use on edible cassava flour and gari
CCMAS44 acknowledged that no amendment to CXS 234 was necessary for the moment, despite some technical elements presented in CCMAS44’s CRD9 document by the International Association for Cereal Science and Technology (ICC) about the revision of ICC Recommendation N. 207, to render it applicable to edible cassava flour and to gari (in particular to include appropriate sieve sizes). CCMAS noted that the ICC revision work was in its final approval stage at ICC level. It was recalled that the current ICC Recommendation N. 207 had already been endorsed by CCMAS43.
SAMPLING PLANS
Information document to the General guidelines on sampling (CXG 50, 2023 version) – e-book with sampling plans applications
CCMAS44 considered the outcome of an inter-sessional EWG chaired by New Zealand and co-chaired by Germany to develop an information document on how implementing the revised Codex Alimenta-rius General guidelines on sampling (CXG 50, 2023 version). Such information document should not be considered as an official Codex text, but simply there to inform countries and food business operators for internal use by CCMAS and other Codex commodity committees. CCMAS44 agreed to publish the revised information document (as presenting in CCMAS44 report’s Appendix IV) and inform Codex committees of the publication of this document. It also agreed to remove the current information document titled “Practical examples of sampling plans” from the Codex website. Finally, it was noted that as other applications (Apps) were being developed, they would be forwarded to the Codex Secretariat for inclusion to the list of applications in the information document and that CCMAS would be informed accordingly. Other supporting resources, such as webinars, would be made available on the CCMAS webpage as well. The agreed information document should also be considered a living document, meaning CCMAS could update it when needed and where warranted [ix].
Review of sampling plans in the general standard for methods of analysis (CXS 234, 2024 version) and development of sampling plans for lots consisting of bulk material/heterogenous lots, including for mycotoxins
CCMAS44 agreed to continue developing the various discussion papers on (a) the review of sampling plans in CXS 234, particularly the various approaches to placing the sampling plans in the standard(s), the format and content of the presentation of sampling plans, and the responsibility for assessing the parameters that determine the selection of the appropriate sampling plan for a given commodity/provision combination; and (b) the development of sampling plans for bulk materials/heterogenous lots, including mycotoxins, including proposed sampling plans for consideration by CCMAS45, and to inform CCCF of this decision. CCMAS44 also noted that work on sampling plans for bulk materials/heterogenous lots, including for mycotoxins, should be conducted in close collaboration with CCCF; and noted the possible need for CCMAS to provide support to commodity committees in their review of sampling plans. CCMAS44 agreed to re-establish an EWG, chaired by New Zealand and co-chaired by Germany to advance the revisions of these discussion papers and prepare a dedicated discussion paper on sampling plans for bulk materials/heterogenous lots, including for mycotoxins, to be discussed by CCMAS45.
OTHER ASPECTS
Numeric performance criteria for the determination of nitrate and nitrite ions in food matrices
CCMAS44 considered the outcome of an intersessional EWG work led by Australia and co-chaired by the USA, including discussions held by the in session VWG. CCMAS44 agreed with the Numeric Performance Criteria (NPC) elaborated (and rounded up during the session) for nitrate and nitrite in three food matrices (i.e., ripened cheeses; processed comminuted meat, poultry, and game products; and, heat-treated processed meat, poultry, and game products in whole pieces of cuts) and agreed to forward these NPC back to CCFA for information. Initial CCFA request was for CCMAS to establish NPC for methods of analysis in these specified food matrices; provide information on available analytical methods suitable for both the adopted MLs and the lowest proposed residue levels; and clarify whether the methods measured nitrate and nitrite ions separately or in combination [x].
Methods of analysis for precautionary allergen labelling
CCMAS44 considered the outcome of an EWG led by the USA and its prior consideration by the IWG. Due to several factors related to the presentation of the list of methods, the need for further consideration, and new method validation guidelines, CCMAS44 agreed to re-establish an EWG chaired by USA and co-chaired by UK to finalize the review of the methods presented at CCMAS 44 against the recently updated CEN and AOAC validation guidelines and performance requirements [xi] and simplify the presentation of the methods and their validation status. CCMAS44 tasked the new EWG to draft a response to CCFL49 for consideration by CCMAS45. CCMAS44 confirmed that the EWG would not have to address the second question from CCFL regarding sampling plans.
Nitrogen to protein conversion factors for commodities approved by Codex Commodity Committees
CCMAS agreed to forward the list of Nitrogen to Protein conversion factors as amended, for approval by CAC48 and future inclusion as an Annex to the General Standard on Methods of Analysis (CXS 234), while noting some inconsistencies with these conversion factors especially for various soy products, and it suggested that these factors should be reviewed in the future. CCMAS44 noted that these factors would need to be reviewed by the relevant Codex Commodity Committees to ensure further consistency [xii].
Harmonization of names and format for principles identified in CXS 234, 2024 version
CCMAS44 considered the outcome of an intersessional EWG work led by Brazil and Chile. Purpose of this work was to (i) establish a centralized database consolidating all methods relevant to CCMAS; (ii) harmonize terminology for analytical methods across Codex standards; and (iii) develop a publicly accessible database on methods of analysis and sampling for inclusion on the Codex website. The work of the EWG to develop harmonized terminology for analytical methods, format for principles and provision names was thus to support the development of such a structured database. CCMAS44 significantly updated the document but was unable to address all the issues. CCMAS44 agreed to re-establish the EWG, led by Brazil and co-led by Chile to further revise the “Harmonization of Names for Principles in CXS 234-1999”, including its annexes A, B, and C, using the text included in CCMAS44 report Appendix VI as its working basis, with the aim of ensuring that the principles in CXS 234 are properly included and continue discussions on Annex D, focusing on separating the provisions into three distinct groups (editorial or no-change provisions, provisions linked to active committees, provisions linked to inactive committees) and making corresponding recommendations [xiii].
Endnotes
[i] Food Production Systems Engineer; Food Standards, Safety and Regulatory Specialist; Counsellor at Keller and Heckman LLP Brussels office
[ii] CCMAS is the specialised body of the Codex Alimen-tarius Commission Food Standard Program dealing with the most complex scientific and technical matters relating to (a) methods of analysis (i.e., analytical chemistry); (b) sampling plans (i.e., statistical analysis) other than those covered by specialised horizontal committees, and (c) any other issues related to these. In addition, CCMAS endorses the methods proposed by Codex Committees developing commodity and food standards. As such, CCMAS outputs are key to help countries and food business operators in performing their conformity assessment to existing Codex food standards, hence ensuring food safety and authenticity of such standardized foods, helping minimizing food fraud, and guaranteeing a better traceability and fair practices in international trade of these food supplies.
CCMAS44 was held virtually through five 3-hour daily sessions from May 5 to 8, 2025 and was preceded by a pre-session virtual working group (VWG) on “Endorsement”, held on April 29 and 30, 2025 and which prepared decisions for CCMAS44 on nearly all agenda items (item 2, 3, 4, 5, 7 and 8). The PWG also continued its work during part of the plenary as an in-session working group (IWG). CCMAS44 adopted its draft report virtually on May 14, 2025. CCMAS44 was attended by 74 Member countries, one Member organization and 21 Observer organizations. The session was chaired by Dr Attila Nagy, Director, National Food Chain Safety Office (NFCSO) and co-chaired by Dr Zsuzsa Farkas, Head of Department, Department of Digital Food Science, University of Veterinary Medicine, Budapest. The next CCMAS meeting (CCMAS45) was tentatively scheduled from 9 to 13 March 2026, to be held in person in Budapest (Hungary) and be preceded by the PWG on “Endorsement” and a regular meeting of the contact group of inter-agencies developing and validating methods of analysis and sampling (i.e., composed of ISO, IDF, AOAC International, FOSFA International, USP-Food Chemical Codex, AACC, ICC, AAFCO, NMKL, ICUMSA, and the international association MoniQA).
[iii] See https://www.fao.org/fao-who-codexalimentarius/ meetings/detail/en/?meeting=CCMAS&session=44&
[iv] See https://www.fao.org/fao-who-codexalimentarius/ meetings/en/
[v] See https://www.fao.org/fao-who-codexalimentarius/ codex-texts/en/
[vi] Adopted methods — Cocoa products and chocolate: Updated methods on fat-free cocoa solids, fat-free milk solids (determined as milk protein), Total Fat (on a dry basis), Cocoa shell (determined as spiral vessel count), cocoa shell (determined as stone cell count). Fish and fishery products (Quick Frozen Fish Sticks (Fish Fingers), Fish Portions and Fish Fillets – Breaded or in Batter – CXS 166 (2017 version)): Fish content (declaration) – Nitrogen, Moisture, Total Fat, Ash. Performance criteria for the methods for sodium chloride and for salt determined as chloride expressed as sodium chloride for boiled dried salted anchovies; fish sauce; salted Atlantic herring and salted sprat; salted fish and dried salted fish of Gadidae family of fishes; Sturgeon caviar. Foods for special dietary uses: Follow up formulas – Vitamin A palmitate (retinyl palmitate), Vitamin A acetate (retinyl acetate), Vitamin A (two AOAC methods), Vitamin E, Vitamin D, Thiamine, Riboflavin, Niacin, Vitamin B6, Vitamin B12, Pantothenic acid, Folic acid, Vitamin C, Biotin, Iron, Calcium, Phosphorous, Magnesium, Sodium, Chloride, Potassium, Manganese, Iodine, Selenium, Copper, Zinc, Total Nucleotides, Choline, Myo-innosi-tol, L-carnitine, Total amino acids (excluding taurine and tryptophan) and Tryptophan both for some selected uses specified in CXS 156 (2023 version), Total fatty acids, Crude Protein, Folic acid (addition of ISO 20631). All Foods: content of insoluble and soluble dietary fibres of higher and lower molecular weight (applicable in food that may, or may not, contain resistant starches (AOAC 2022.01/AACC 32-61.01/ICC Standard n° 191 as type I method) with note relating to the subtraction rule resulting from Codex definition of dietary fiber as deemed appropriate by the competent authority. Fruit juices and nectars: L-Ascorbic acid (4 methods), Citric acid (all uses), High Fructose Corn Syrup and Hydrolyzed Inulin Syrup (in apple juices as permitted ingredients), L-Malic Acid, Saccharin, Soluble solids, Sucrose, Phosphorous/Phosphate. Milk and milk products:amendment to the commodity standard on the moisture content to add whey powders to the list, Numeric Performance Criteria for methods used for the quantification of Copper and Iron. Miscellaneous products -Dried Meat: Chloride as sodium chloride; Food Grade Salt: Iodine (only for products fortified with Iodate) and Sodium Chloride and description of the determination of sodium chloride and related sampling method for food grade salt.
Revoked methods — Fish and fishery products (Salted Fish and Dried Salted Fish of the Gadidae Family of Fishes – CXS 167 (2018 version): Determination of salt content, Salt saturation. Follow up formulas: Vitamin A by colorimery (AOAC 974.29, Type IV), Iodine (milk-based formula, AOAC 992.224 by Ion selective potentiometry). All foods: previously mentioned methods for dietary fibers (AOAC 2011.25 and AACC Intl 32-50.1). Fruit Juices: Carbon dioxide (additives and processing aids) by IFU n°42, Malic acid by EN 1138.
Unchanged methods — Cereals, Pulses and Legumes and derived products: Quinoa – protein content (type IV) until further work discussed. Fruit Juices and Nectars: Malic acid (additives); Preservatives in fruit juices (sorbic acid and its salts). Milk and milk products: Whey powder — Water (moisture) noting that the water content is excluding the crystallized water which is bound to lactose (that part being generally known as the moisture content). Dried meat: Chloride as sodium chloride (≥ 0.25% or ≥ 1.0%).
Methods for further consideration until CCMAS45 with some amended during the IWG/CCMAS44 sessions – Chocolate and Chocolate Products: Cocoa butter (determined as fat); Milk fat; Moisture; Moisture (Determined as Water); Non-cocoa butter vegetable fat; Fat; Free fatty acids; Unsaponifiable matter; Cocoa butter equivalents in cocoa butter and plain chocolate; Cocoa butter Equivalents in Milk Chocolate; Determination of center and coating of filled chocolate (all methods approved for the chocolate type used for the coating and those approved for the type of center concerned). Cocoa powders (cocoa) ad dry cocoa-sugar mixtures: Moisture (Determined as Water); Determination of full-fat cocoa powder, fat-reduced cocoa powder, and highly fat-reduced cocoa powder; Determination of cocoa butter (to be developed). Follow-up formula: Riboflavin, Niacin (x2), Vitamin B6 (x2), Vitamin B12 (x2), Folic acid (x2), Biotin, Iron (x2), Calcium (x2), Phosphorous, Magnesium (x2), Sodium, Chloride, Potassium, Manganese, Selenium (x4), Copper, Zinc, Choline. Fruit juices and nectars: Benzoic acid and its salts – Sorbic acid and its salts, Benzoic acid and its salts, Sulphur dioxide alts, Sulphur dioxide (x3), Tartaric acid in grape juices, Total Nitrogen, Acetic acid (acetate), Alcohol (ethanol), Anthocyanins, Ash, Beet sugar, Benzoic acid, C13/C12 ratio of ethanol derived from fruit juices, Carbon stable isotope ratio (x2), Carotenoids (as total carotenoids and as individual groups), Centrifugable pulp, Chloride (expressed as sodium chloride), Chloride, Essential oils, Essential oils in citrus fruit, Fermentability, Formol number, Free amino acids, Fumaric acid, Glucose Fructose and Sucrose/Saccharose, Glycerol, Hesperidin and Naringin (x2), Hydroxymethylfurfural (x2), D-isocitric acid (x2), D- and L- Lactic Acid, L-Malic/Total Malic ratio to detect added D-Malic acid, pH value (x2), Proline, Relatice density (x2), Sodium Potassium Calcium and Magnesium, D-Sorbitol, Starch, Titratable acids, Total dry matter at 70°C, Total solids (by microwave oven drying), Vitamin C (dehydro-ascorbic acid and ascorbic acid). Fruit juices: Carbon stable isotope ratio of sugars from fruit juices. Apple Juice: High Fructose Corn Syrup and Hydrolyzed Inulin. Orange juice: Sugar beet derived syrups in frozen concentrated orange juice.
[vii] See https://ifu-fruitjuice.com/page/LCHP2
[viii] CCMAS44 recalled that CCMAS43 endorsed the method for determining protein in quinoa (ISO 1871) as Type IV, noting that the typing could be reconsidered should more information be provided. The VWG considered replies to CL 2024/91-MAS, but information provided at that time of the IWG met did not allow the VWG to find any consensus on retyping the ISO 1871 method as a type I method. During the VWG, another method was also offered as an alternative Type I method for the determination of protein in quinoa (i.e., ISO 20483), but it was noted a lack of specific validation data of that method for pseudocereals such as quinoa. The ISO representative informed the VWG that quinoa could be added in future as a validated matrix and that ISO might consider taking up that work if needed (based on an ISO member internal request and ISO working procedures). CCMAS44 extensively discussed the information submitted by seven countries from Latin America (Bolivia, Peru, Ecuador, Colombia, Chile, Uruguay, and Argentina), as presented in CCMAS44’s CRD19 document. Such information was recognised to be supportive of a retyping of the method ISO 1871 as Type I (official method). Information in CRD19 informed CCMAS44 on details about the validation studies and process, the reagents used, the conditions of the methods, the catalysts used, while noting that a single reference material for quinoa was also used during the validation studies. An explanatory footnote was proposed (e.g. regarding conditions, the catalysts and reagents used), noting that the same footnote would be consequentially applied to the ISO 1871 method for determining protein in Tehena to ensure consistency. It was also reiterated that CCMAS should apply the same decisions regarding the use of ISO 1871 for the determination of protein to Tehena to ensure consistency. Members and Observers which did not support the proposal expressed concerns that ISO 1871 was a general guidance and not a step-by-step method, since it did not specify conditions and chemicals. In accordance with the definition for a Type I method, a detailed analysis of the steps taken across the different validation studies would be necessary to retype ISO 1871 from Type IV to Type I, even though there was no issue with the validation data themselves. CCMAS44 agreed that this topic should be deferred to the PWG on endorsement that would meet immediately prior to CCMAS45 to allow more time to review CRD19.
[ix] The document provides additional information about the sampling plans referred to in the CXG 50, by providing examples for each of the main types of sampling plans, additional information on other sampling plans, including Bayesian plans, and links to the Apps for designing and evaluating such sampling plans. App 1 evaluates and designs sampling plans for homogeneous lots, which is included in the information document by link. Apps 2 and 3 were being developed and would be included in the information document once available. As more Apps are developed, links to these Apps would be included also in the information document. Other resources (e.g. video clips, webinars) would be provided to the extent possible on Codex website (such as the one held on April 28, 2025). As recommended during the two previous CCMAS sessions on this matter for including sampling plans involving smaller sample sizes or less testing, part 3 of the document includes presentation of Bayesian plans, based on risk- or utility-based approaches, while the overall rest of the document structure remained largely unchanged. CCMAS44 discussed an edited version of the information document, as included in CCMAS44’s CRD35. Some concerns were expressed by Japan about the inclusion of Bayesian plans in the information document, as the scope of current CXG 50 (2023 version) was restricted to acceptance sampling plans for inspecting isolated homogeneous lots (i.e., and therefore not using Bayesian approaches). It was clarified that Bayesian sampling plans provided a potential way to reduce testing costs and was an area of still on-going international scientific work, including within ISO, about which a technical report on applying Bayesian methods to acceptance sampling was expected to be published end 2025. It was also suggested that the information document may need to be complemented with information relating to the Codex Principles for the Use of Sampling and Testing in International Food Trade (CXG 83, 2015 version).
[x] CCMAS44 noted the NPC were developed for both adopted MLs and the lowest proposed residue levels in the relevant food matrices. It also reviewed the list of methods submitted by CCFA, including one recently published method added and provided a summary of the method validation data (in Appendix 3 of CCMAS44 working document CX/MAS 25/44/10) for assessment against the NPC. “Examples of applicable methods that met the established criteria” that met the NPC had been identified from Appendix 3 and were presented in Appendices 1 and 2 of CX/MAS 25/44/10. The revised versions were therefore presented in Appendix VI of CCMAS44 CRD02 Rev.1. It was highlighted that should CCFA decide to revise the lowest proposed residue levels, suitable analytical methods should be selected based on the information provided in Appendix III of CCMAS44 working document CX/MAS 25/44/10.
[xi] (a) Dr. Latimer, George W, Jr. (ed.), ‘Validation Procedures for Quantitative Food Allergen ELISA Methods: Community Guidance and Best Practices’, in Dr. George W Latimer, Jr. (ed.), Official Methods of Analysis of AOAC INTERNATIONAL, 22nd Edition (New York, 2023; online, AOAC Publications, 4 Jan. 2023). (b) EN 17855:2024 Foodstuffs – Minimum performance requirements for quantitative measurement of the food allergens milk, egg, peanut, hazelnut, almond, walnut, cashew, pecan nut, Brazil nut, pistachio nut, macadamia nut, wheat, lupine, sesame, mustard, soy, celery, fish, mollusks and crustaceans, CEN, 2024.
[xii] The proposed conversion factors for adoption were included in Appendix III of the CCMAS44 report. Nitrogen To Protein Conversion Factors For Commodities Approved By Commodity Committees Proposed For approval by CAC48 and Future Inclusion as an Annex to CXS 234: Animal Protein Source: Milk and milk products – 6.38; Meat and meat products – 6.25. Infant formula: The calculation of the protein content of infant formulas prepared ready for consumption should be based on N x 6.25, unless a scientific justification is provided for the use of a different conversion factor for a particular product. The value of 6.38 is generally established as a specific factor appropriate for conversion of nitrogen to protein in other milk products, and the value of 5.71 as a specific factor for conversion of nitrogen to protein in other soy products. Follow-up formula for older infants and product for young children: The calculation of the protein content of the final product ready for consumption should be based on N x 6.25, unless a scientific justification is provided for the use of a different conversion factor for a particular product. The protein levels set in this standard are based on a nitrogen conversion factor of 6.25. For information the value of 6.38 is used as a specific factor appropriate for conversion of nitrogen to protein in other Codex standards for milk products. In accordance with the Guidelines on nutrition labelling (CXG 2-1985), the calculation of protein for nutrient declaration purposes should be based on a conversion factor of 6.25, unless a different factor is specified in the present annex. Fish and fishery products: Crackers from marine and freshwater fish, crustaceans and molluscan shellfish – 6.25. Plant Protein Source: Wheat, wheat protein products – 5.71; Maize – 6.25; Quinoa – 6.25; Sorghum – 6.25; Millet (grains and flour) – 5.71; Gochujang – 6.25. Soya and non-fermented soybean products: 5.71; Tempe – 5.71; Natto – 5.71; Cheonggukjang – 5.71. Vegetable protein Products (VPP): Products produced by separation from wheat and soya grains and flours of certain non-protein constituents (starch, other carbohydrates) – 6.25. Soy protein products – 6.25. CCMAS44 noted that the list would continue to be updated as new nitrogen to protein conversion factors were agreed by commodity committees. It was also explained that in cases where such nitrogen to protein conversion factors had been developed by a committee adjourned sine die (or dissolved) and needed further review, the Codex Secretariat would look into some practical modalities for such a review.
[xiii] The document included in Appendix VI of CCMAS44 report is entitled “Harmonization of Names for Principles in CXS 234-1999” is composed of the following sections: 1. General Guidelines; 2. Definitions (Principle, Biological assay, Chromatography, Colorimetry, Gravimetry, Potentiometry, Sensory assay, Spectroscopy, Mass Spectrometry (MS), Titrimetry, Visual examination, Volumetry); 3. Criteria Used (3.1. Assays Whose Results are Method Dependent – e.g., Moisture at 105°C – Gravimetry, etc.; 3.2 Assays Whose Results are independent of the method – e.g., Nitrate – UV-Vis (ultraviolet visible) – Spectrophotometry, etc.); 4. Additional information (to consider removing any additional information such as “ashing”, “ceramic filter filtration”, etc.); Annex A — Principles of Methods of Analysis (e.g.; Anodic Stripping Voltammetry (ASV), etc.); Annex B – Acronyms and abbreviations (e.g., AAS Atomic Absorption Spectrophotometry; etc.); Annex C List of Acronyms for Standard Method References (e.g., AACC, USP, ISO, etc.); and the to-be-developed Annex D – List of Provisions. CCMAS44 also noted the view that the provisions in CXS 234 should remain aligned with those in the commodity standards to avoid misalignment and confusion. It was further emphasized that the provisions in CXS 234 reflected the original commodity standard provisions and should not be oversimplified as this could remove essential context. Some provisions indicated method complementarity and had been the subject of extensive discussions. Some of the proposed changes in Annex D carried significant implications. Therefore, consultation with commodity committees and other relevant committees was necessary and for better clarity future proposed changes would be presented in three groups: those requiring no changes or only editorial changes; those changes linked to active commodity committees; and those changes related to adjourned sine die or abolished commodity committees. The Codex Secretariat also clarified that, in general, CCMAS did not have the authority to make such changes to provisions falling within the remit of a Commodity Committee adjourned sine die (or abolished/dissolved). If necessary, such proposals should be referred to the CAC, as per the mechanism followed precedingly with the proposed amendment of a provision in section 3.3 of the Codex Standard for Edible Casein Products (CXS 290).
GLP-1 Compounded Medications Targeted by Connecticut Attorney General
On May 21, 2025, the Connecticut Office of the Attorney General released a statement and sent letters to Connecticut weight loss clinics, med spas, medical practices and other businesses regarding allegedly or potentially unfair and deceptive conduct relating to compounded GLP-1 medications. Specifically, healthcare providers in Connecticut that advertise and prescribe compounded GLP-1 medications, such as semaglutide and tirzepatide, may be considered to be violating the Connecticut Unfair Trade Practices Act (CUTPA).
The Attorney General provided several reasons for why providers advertising and prescribing compounded semaglutide and tirzepatide may be violating CUTPA:
Compounding pharmacies are no longer allowed to manufacture semaglutide and tirzepatid injections in bulk (meaning copies of commercially available, U.S. Food and Drug Administration (FDA)-approved GLP-1 semaglutide and tirzepatide products), as they have been removed from the FDA’s shortage list. (More information can be found in Foley’s article “GLP-1 Drugs: FDA Removes Semaglutide from the Drug Shortage List”),
The FDA has raised health and safety concerns about these compounded medications, citing issues such as dosing errors, poor inspection records from overseas manufacturers, and, in some instances, adverse events, some of which required medical intervention,
These compounded medications are often inaccurately labeled as “generic” versions of semaglutide and tirzepatide injections and may contain additives, such as vitamins, which have not been approved by the FDA or evaluated through clinical trials, and
The FDA has not approved any oral GLP-1 medications, nor has it approved the use of GLP-1 medications for cosmetic purposes.
The Connecticut Attorney General has put providers on notice and stated he is prepared to take appropriate action against businesses and individuals who continue to advertise and prescribe semaglutide and tirzepatide in violation of CUTPA.
Weight loss clinics, med spas, medical practices and other businesses advertising and prescribing compounded versions of semaglutide and tirzepatide in Connecticut are advised to come into compliance with the CUTPA.
Special thanks to Alina Mueller, a summer associate in Foley’s Denver office, for her contributions to this article.
This Week in 340B: May 27 – June 2, 2025
Find this week’s updates on 340B litigation to help you stay in the know on how 340B cases are developing across the country. Each week we comb through the dockets of more than 50 340B cases to provide you with a quick summary of relevant updates from the prior week in this industry-shaping body of litigation.
Issues at Stake: Other; Contract Pharmacy; HRSA Audit Process; GPO Prohibition
In a case against the Health Resources and Services Administration’s (HRSA) challenging its certification of a group of entities as 340B-eligible, the government filed a reply in support of its partial motion to dismiss.
In a case by a covered entity challenging the government’s decision to allow a manufacturer’s audit, the government filed a motion to dismiss.
In a case by a covered entity against the government, the court granted the covered entity motion for leave to file a response to the intervenors’ amicus brief.
A drug manufacturer filed a complaint challenging a Hawaii state law governing contract pharmacy arrangements.
In a case challenging HRSA’s policy limiting the circumstances in which covered entities can use their group purchasing arrangements to purchase non-340B drugs, the plaintiff filed a combined reply in support of its motion for summary judgment and opposition to defendant’s cross motion for summary judgment.
In three cases challenging state laws in Tennessee, South Dakota, and Nebraska governing contract pharmacy arrangements:
Tennessee: The defendant filed a response in opposition re motion for preliminary injunction.
South Dakota: The plaintiff filed a memorandum in opposition to defendant’s motion to dismiss.
Nebraska: The defendant filed a reply to plaintiff’s brief in opposition to defendant’s motion to dismiss.
Federal District Court Upholds Authority of HHS to Pre-Approve 340B Rebate Programs; HRSA Submits Proposed 340B Rebate Guidance
A federal judge in D.C. recently ruled in favor of the U.S. Health Resources and Services Administration (“HRSA”), an administrative agency under the U.S. Department of Health and Human Services (“HHS”), by finding that drug manufacturers must obtain pre-approval from HRSA before implementing rebate models under the 340B Program. Specifically, U.S. District Judge Friedrich (“Friedrich”) found that HHS and HRSA did not exceed their authority when they required Eli Lilly & Co., Bristol Myers Squibb Co., Sanofi-Aventis U.S. LLC, Novartis Pharmaceuticals Corp. (“Novartis”) and Kalderos Inc., a health care tech company (together, the “Companies”) to seek pre-approval of the rebate plans they offered.[i]
Cases Impacted by the Decision
The five separate lawsuits on which Friedrich ruled involve claims from the Companies that HHS illegally blocked their efforts to implement rebate models instead of offering up-front drug price discounts to 340B covered entities. Friedrich held that the 340B statute “contemplates that the Secretary may ‘have as a condition’ or ‘stipulate’ how any rebate or discount is accounted for in the price ultimately paid by [340B] covered entities. That plain text provides authorization for [HRSA] to regulate the implementation of price reductions.” Friedrich further found that HHS and HRSA did not act arbitrarily and capriciously by requiring the Companies to get their rebate plans pre-approved before implementing them.
Origin of the 340B Rebate Disputes
Last year, Johnson & Johnson Health Care Systems Inc. (“J&J”) proposed that hospitals should pay full price for two popular J&J medications, and then file a claim for a rebate in order to receive the discounts to which the hospitals are entitled under the federal 340B program. Following objections from HRSA officials and hospitals, J&J reportedly ceased “implementation of its 340B rebate proposal” and last November, J&J sued HHS and HRSA.[ii] Manufacturers have taken the stance that a rebate model is permitted by the 340B statute and that the rebate model provides better control and protection against duplicate discounts. [iii] Advocates opposing the rebate model argue that the 340B statute does not permit a retroactive discount and that the rebate model would create significant financial and operational hurdles for safety net hospitals and other entities participating in the 340B Program. [iv]
What’s Next?
While the ruling is considered a temporary win for 340B covered entities, Friedrich did not conclude that rebate models are prohibited under the 340B statute. At the time of the ruling, HRSA had only formally rejected Sanofi-Aventis’s rebate model, while the others remain pending a final decision from HRSA. As to Sanofi, Friedrich ruled that HRSA had not provided adequate justification for its denial of the rebate model and ordered HRSA to reconsider Sanofi’s proposal. On June 1, 2025, HHS and HRSA submitted their proposed 340B Rebate Guidance to the Office of Management and Budget for regulatory review, It is unclear when the review will be finalized and made available to the public. Once the guidance is released, 340B covered entities should determine how it may affect their operations and consider consulting with their 340B attorneys on navigating any new requirements or implications.
FOOTNOTES
[i] Eli Lilly & Co. et. Al. v. Robert F. Kennedy Jr. et al., (Case No. 24-cv-03220); Bristol Myers Squibb Co. v. Robert F. Kennedy Jr. et al., (Case No. 24-cv-03337); Sanofi-Aventis U.S. LLC v. Robert F. Kennedy Jr. et al., (Case No. 24-cv-03496); Novartis Pharmaceuticals Corp. v. Robert F. Kennedy Jr. et al., (Case No. No. 25-cv-00117); and Kalderos Inc. v. Robert F. Kennedy Jr. et al., (Case No. 21-cv-02608).
[ii] See American Hospital Association, J&J sues government over 340B proposal; AHA says J&J’s legal arguments ‘completely meritless’ (Nov. 13, 2024).
[iii] Craig Clough, Feds Get Early Win In Drugmakers’ Suit Over 340B Rebates (May 19, 2025).
[iv] Amicus Curiae Brief of American Hospital Association, National Association of Children’s Hospitals, Inc., d/b/a Children’s Hospital Association, Association of American Medical Colleges, and America’s Essential Hospitals in Support of Defendants, Eli Lilly & Co. v. Kennedy, Nos. 24-cv-3220, 24-cv-3337, 25-cv-0117 (DLF) (D.D.C. filed Mar. 4, 2025), ECF No. 31-1.
Listen to this post
Quantum Computer Hardware: How Quantum Computers Are Implemented
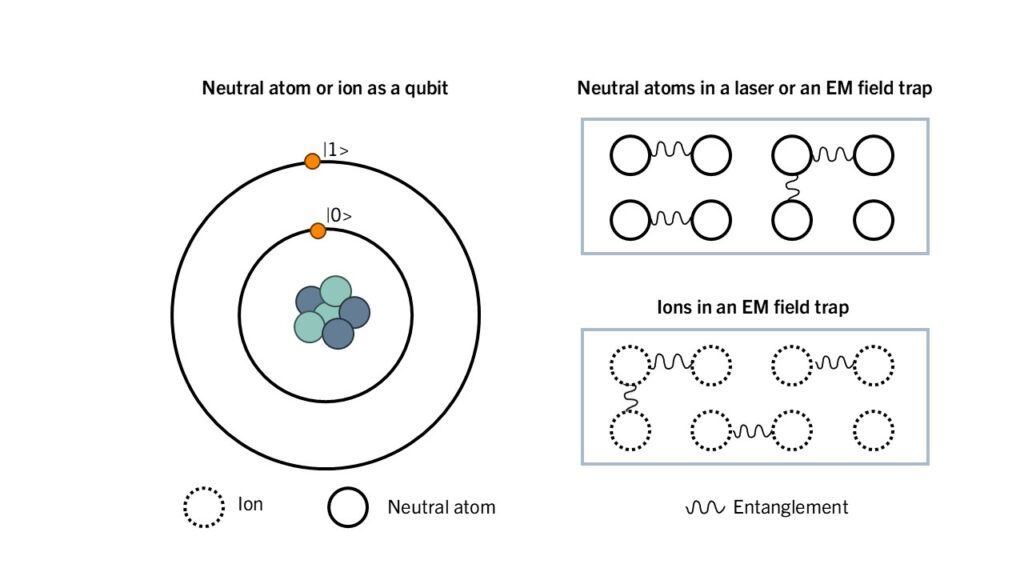
In the previous article titled “The Basics: How Quantum Computers Work and Where the Technology is Heading,” we provided an overview of foundational quantum computing concepts, including qubits (quantum bits), superposition, and entanglement. Building on these principles, in this article we will provide an overview of how qubits are implemented in real, physical systems to make quantum computing possible. There are many leading approaches to quantum hardware design, each with different techniques for maintaining qubit stability and minimizing decoherence. Among them, promising approaches include (1) neutral atom quantum computers, (2) trapped ion quantum computers, (3) superconducting quantum computers, and (4) spin qubit quantum computers. We explore the underlying physical systems of each approach, discussing their advantages and trade-offs, while recognizing that the development of each creates different implications.
Neutral Atom Quantum Computers
Neutral atom quantum computers operate using lasers or electromagnetic fields to trap neutral atoms in a localized region. In such systems, neutral atoms serve as qubits by storing quantum information in the energy levels of the atoms’ electrons or hyperfine states of the atoms. The internal states of the neutral atoms serve as the logical |0⟩ and |1⟩ states of the qubits.
Precisely controlled laser or electromagnetic pulses are used to manipulate the neutral atoms to initialize the qubits, carry out quantum operations, and perform measurements of their quantum states. Single-qubit operations can be achieved by applying tuned laser or electromagnetic pulses to couple two selected internal energy levels of a single atom. The duration, frequency, and intensity of the pulses can be adjusted to change the qubit’s state from |0⟩ or |1⟩, or any superposition in between, to perform different gates with the single atom.
Neutral atom quantum computers can implement two-qubit gates by leveraging the “Rydberg blockade” effect. To do so, lasers or electromagnetic pulses are used to excite a qubit to a high-energy state known as the “Rydberg state.” When shifting to this high-energy state, the excited atom shifts the energy levels of neighboring atoms, preventing those neighboring atoms from being excited to similar energy states. The Rydberg blockade effect can be used to establish superposition between two neighboring atoms, producing multi-qubit gates.
Advantages of neutral atom quantum computers include high scalability and uniform qubit characteristics through large arrays of common atoms. Laser and electromagnetic pulses also provide precise control over qubit states. However, trapping and stabilizing neutral atoms is challenging because minor misalignments or power changes in the laser beams can cause atoms to drift or escape. Additionally, all neutral atoms must be maintained in a controlled vacuum environment to prevent decoherence due to collisions with background gases.
Trapped Ion Quantum Computers
In contrast to neutral atom quantum computers, trapped ion quantum computers confine (e.g., immobilize) charged atomic particles (ions) in free space using electromagnetic fields. Motion of each trapped ion is mitigated by laser-cooling the ions to near their ground state. Like neutral atom quantum computers, each atom in a trapped ion system operates as a qubit that encodes quantum information in the electronic or hyperfine states of each ion (e.g., using laser or microwave pulses).
Multi-qubit operations are realized in trapped ion quantum computers by coupling the ions’ internal qubit states to shared vibrational modes between proximate ions. As the ions are trapped within the electromagnetic field, any vibrational motion of one ion (e.g., induced via laser pulses) causes multiple ions to exhibit quantized motion through Coulomb interactions (i.e., electromagnetic repulsion between the charged ions). With precisely controlled laser or electromagnetic pulses, the induced vibrations can cause selected ions to become entangled, allowing for various multi-qubit gates and quantum operations.
Trapped ion quantum computers have several advantages, including low error rates with long coherence times, high-fidelity quantum gates, extensive possible arrangements of entangled particles (i.e., with each ion in a trap capable of being entangled with any other ion in the trap), along with well-understood and standardized gate schemes that facilitate straightforward implementation of quantum algorithms.
However, these systems typically involve slower processing times compared with systems that use solid-state qubits (e.g., superconducting circuits or silicon-based qubits). Additionally, trapped ion systems typically require complex laser and electromagnetic infrastructure to achieve useful results. Like neutral atom systems, trapped ion systems require controlled vacuum conditions to prevent decoherence due to collisions with background gases or other particles.
Superconducting Quantum Computers
Superconducting quantum computers leverage the properties of superconducting materials to create and control qubits. Superconducting materials, or “superconductors” are materials that can conduct electricity with no resistance or energy loss. Superconductors operate at extremely low temperatures, typically within a few kelvins of absolute zero (e.g., 1 to 20 K or -272 to -253°C). Superconducting quantum computers use a superconductor structure called “Josephson junction” to implement superconducting qubits (e.g., superconducting electronic circuits).
Josephson junctions are thin, insulating barriers positioned between superconducting materials, which can be used to create a variety of different qubits, including transmon qubits and flux qubits. Transmon qubits are created by connecting a Josephson junction in parallel with a relatively large capacitor. This creates a non-linear LC oscillator, which enables the creation of discrete energy levels to implement quantum computing. Quantum information can be encoded in the energy states of transmon qubits using microwave pulses, which induce transitions between the discrete energy levels of the qubit. Transmon qubits can be entangled using capacitive coupling or inductive coupling of adjacent qubits, or through coupling to a common resonator, such as a microwave cavity or transmission line.
On the other hand, flux qubits are formed using a “superconducting loop,” or current path, that includes one or more Josephson junctions. Flux qubits encode quantum information in the magnetic flux of each qubit, mediated by the direction of current through the superconducting loop. The current directions (e.g., clockwise or counterclockwise) serve as the logical |0⟩ and |1⟩ states of the qubits. Flux qubits are controlled using a combination of external magnetic flux tuning and electromagnetic pulses. More specifically, the pulses and magnetic flux can be used to externally adjust the state of the qubit, inducing transitions between |0⟩ and |1⟩ states and implementing single-qubit gates. Multi-qubit gates can be achieved through entangling flux qubits via inductive coupling of adjacent qubits, shared Josephson junctions, or coupling to common resonators.
Implementing quantum computers using superconductors has a number of benefits, including very fast gate operations and the ability to manufacture such systems using lithographic techniques that are similar to those used to manufacture conventional semiconductor circuits. Superconducting quantum computers are also easy to scale due to their ease in manufacturing, and benefit from a well-established research community. However, superconducting suffers from limited coherence times and can only operate at ultracold temperatures. Such systems are also susceptible to noise, particularly from crosstalk produced from electromagnetic pulses used to control individual qubits.
Spin Qubit Quantum Computers
Spin qubit quantum computers implement spin qubits, which encode quantum information within the spin of charge carriers (e.g., electrons) in semiconductor materials. Spin is a quantum property of subatomic particles that can be in a superposition of up or down, which can respectively represent the logical |0⟩ and |1⟩ states of the qubits. Quantum information of each electron (e.g., spin-up and spin-down states) can be controlled by rotating the spin of an electron in “quantum dots.” Quantum dots are regions within the semiconductor material that confine electrons in all three spatial dimensions. In some systems, donor atoms implanted in semiconductor material, such as atoms of phosphorous implanted within a silicon substrate, can be used to isolate the spin of electrons.
Spin qubits can be controlled using a variety of optical, electromagnetic, or thermal techniques. In some systems, single-qubit gates can be implemented by controlling the state through the application of an oscillating magnetic field tuned to the frequency of the target qubit. Oscillating electric fields may also be used to transition the spin of one or more qubits to a desired state.
Multi-qubit gates can be implemented by providing a tunnel barrier between two quantum dots or donor atoms. The interaction between spins causes the two adjacent electrons to become entangled, which can be used to create gates. The multi-qubit gates can be controlled by applying a voltage across the gate, which affects how the spins of the adjacent electrons interact.
Spin qubit quantum computers have a number of advantages, including long coherence times, small footprint, and compatibility with existing semiconductor manufacturing processes. However, such approaches still require extremely low temperatures to operate (e.g., near absolute zero). Additionally, spin qubit quantum computers suffer from poor scalability due to complex circuitry required to precisely route high-frequency voltage signals to each qubit within the system.
Nitrogen-Vacant Qubits
A promising new paradigm in quantum computing leverages nitrogen-vacancy (NV) centers in diamond to create robust, room-temperature qubits. NV centers are atomic-scale defects in the diamond lattice, consisting of a nitrogen atom adjacent to a vacancy, which exhibit spin-dependent photoluminescence and exceptionally long spin coherence times. These properties allow the NV centers to function as potentially highly stable qubits that can be initialized, manipulated, and read out optically or through microwave fields. Unlike many other quantum systems that require extreme cooling, NV center qubits maintain quantum coherence even at room temperature, opening the door to more practical and scalable quantum devices. Additionally, their sensitivity to magnetic, electric, and thermal environments enables advanced quantum sensing applications alongside quantum computation. This diamond-based approach combines biocompatibility, durability, and potential for integration with existing semiconductor technology, making it a strong candidate for the next generation of quantum technologies.
The Implications
These quantum computing approaches or implementations have different technological advantages, timelines for maturity and commercial readiness, supply chains, potential strategic partnerships, use cases, product impacts, costs, etc., as suggested. Understanding the various implications will be important for assessing impact, strategic and otherwise. As the race for quantum supremacy and for consumer-grade quantum computing intensifies, it will shape investments, strategic decisions, business timelines, and risk analysis. While it is too early to ascertain which approach(es) may achieve dominance, now is the time for strategists, analysts, and decision-makers to become familiar with the candidates.
Makary Says Psychedelics Are Maybe Okay, M’Kay?
Drugs are bad, m’kay. But what if they’re not? Psilocybin continues to be in the limelight for its potential medicinal uses, including most particularly its potential to combat the nation’s growing mental health crisis. Last week, we reported on the fact that President Trump’s surgeon general nominee was a potential proponent of the use of psychedelics like psilocybin. Now, another member of Trump’s administration has chimed in, and this time it’s someone from the Food and Drug Administration.
The head of the FDA has advised that “exploring the therapeutic potential for psychedelics such as psilocybin and ibogaine is a top priority for the Trump Administration.” According to FDA Administrator Matt Makary, who spoke on News Nation recently,
When it comes to some of these psychedelics and other plant-based therapies, I don’t think we’re listening to patients… I don’t think the medical establishment is listening to doctors. When I listen to the individuals who have tried some of these for real medical conditions—post-traumatic stress disorder, severe refractory depression—people tell me that they believe that psilocybin was successful. It was a curative, or significantly helped, their severe mood disorder.
People have told me that other psychedelics, like MDMA, have been helpful in treating PTSD. Doctors have told me that they’ve sent patients for this therapy… Ibogaine has been used to treat PTSD. There are trials now looking at it for traumatic brain injury—things we have had nothing for in the past. What have we had to treat traumatic brain injury and PTSD that has really had great results up until this time?
To be sure, Makary has said he is not necessarily endorsing these plant-based medicines but does think it’s important to be sure the FDA doesn’t “get in the way with red tape.”
We’ve become used to seeing administrative and executive officials, including the VA and members of Congress, acknowledging the potential benefits of psychedelics as medicine. But last year, under a different administration, FDA dealt a significant blow to the industry, deciding not to approve Lykos Therapeutics, Inc.’s MDMA-assisted PTSD therapy. Makary’s recent statements may mean a sea change for the FDA. We think it’s likely that companies supporting psychedelics research will be emboldened and may become more aggressive in seeking trials and approval under this administration. But much remains to be seen, and Makary has definitely left himself with plenty of ways out. Stay tuned.
Listen to this post